STUDY: The Potential Impact of a Medicare Public Option on U.S. Rural Hospitals And Communities
A new study by Navigant Consulting, Inc. reveals that the “public option,” a new government health insurance system outlined in several current proposals, could put more than 1,000 rural American hospitals in 46 states “at high risk of closure.”
These are the facts:

High Risk for Rural Hospitals
As many as 55% of rural hospitals, or 1,037 hospitals across 46 states, could be at a high risk of closure under the public option. With rural hospitals already under significant strain, a new government insurance system would have drastic consequences for the availability of high-quality care.
If employers shift between 25% and 50% of their covered workers from commercial coverage to a Medicare public option, hospital revenues are projected to drop between 8% and 14% and cause an estimated 51% to 55% of rural hospitals to face high risk of closure, with an additional 39% to 41% facing moderate risk.


Under a new one-size-fits-all government insurance system, hospital revenues are projected to drop between 8% and 14%, meaning fewer hospital employees to treat and house patients, and decreased capacity to provide the high-quality care Americans deserve.
How many rural hospitals could be put at HIGH risk of closure in your state?
Currently, across the country, rural hospitals face budget cuts, reductions in services, and even closures. Rural hospitals are already at risk. A new government-run insurance system like the public option would compound the issues plaguing rural hospitals around the nation, forcing even more to close their doors.
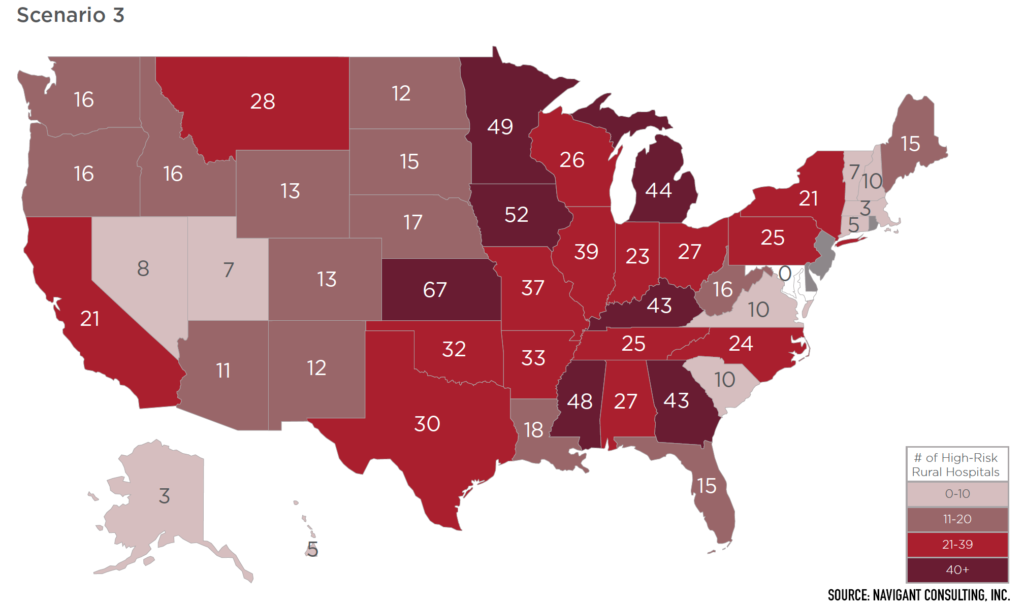
Learn more about the impact in your state here.
Here’s the Truth:
Rural hospitals have faced cuts for years, causing reductions in their ability to provide specialty care like OB-GYN units, NICU facilities and more. A recent report from the Kaiser Family Foundation highlights this issue, finding that “hospital closures reduced local residents’ access to care (especially emergency care), led to an outmigration of health care professionals, and worsened pre-existing challenges in obtaining access to specialty care.”
These troubling predictions about the public option resemble those surrounding Medicare for All, as The New York Times reports that experts are sounding alarm bells about the “violent upheaval” it would cause hospitals: “Some hospitals, especially struggling rural centers, would close virtually overnight, according to policy experts. Others, they say, would try to offset the steep cuts by laying off hundreds of thousands of workers and abandoning lower-paying services like mental health.”
A risky proposal like Medicare for All would upend our healthcare system as we know it instantly – but over time, similar proposals like the public option would inflict the same damage to Americans’ access to high-quality care.
The implementation of a public option on health exchanges presents significant risks to rural hospitals and communities nationwide. Even with a conservative estimate, the public option would exacerbate the already significant financial risks rural hospitals face. If a substantial percentage of the commercial population were to shift to reimburse at Medicare rates, a large proportion of high-risk hospitals would see a grave threat to their viability, and hundreds of rural hospitals presently at lower levels of risk would move to the high-risk category.